While anyone can develop this type of hernia, it's more common in people 50 and over.
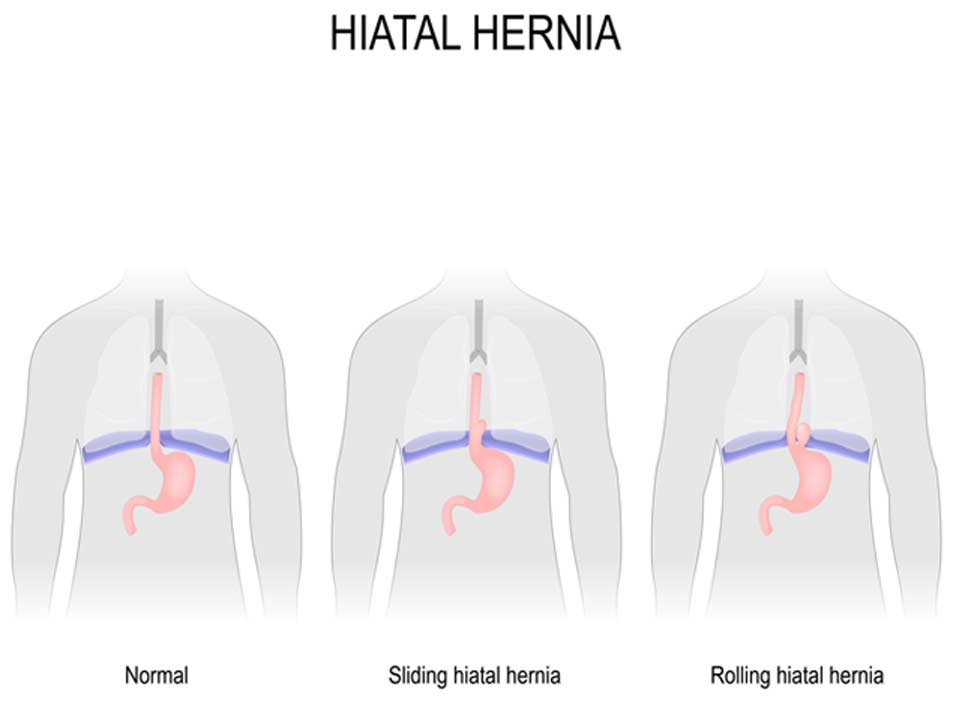
When the upper portion of the stomach pushes through a large muscle called the diaphragm into the chest area, it’s referred to as a hiatal hernia. The stomach is normally located below the diaphragm. But this is not the case when a weak spot allows the stomach’s position to change.
Hiatal Hernia Causes and Symptoms
A hiatal hernia is caused by weakened muscle tissue. Some people get this type of hernia because of injury, while others may naturally have thin diaphragm tissue in the thoracic cavity due to genetic defects or other abnormalities. Vomiting, a chronic cough, and repetitious strain within the upper stomach/lower chest area are possible factors that could contribute to the formation of a hiatal hernia. Smaller hernias of this type may produce little or no symptoms. It’s usually mid-size and larger hiatal hernias that result in noticeable symptoms that may include:
- Heartburn that gets worse when resting or lying down
- Epigastric or chest pain
- Frequent belching
- Trouble swallowing
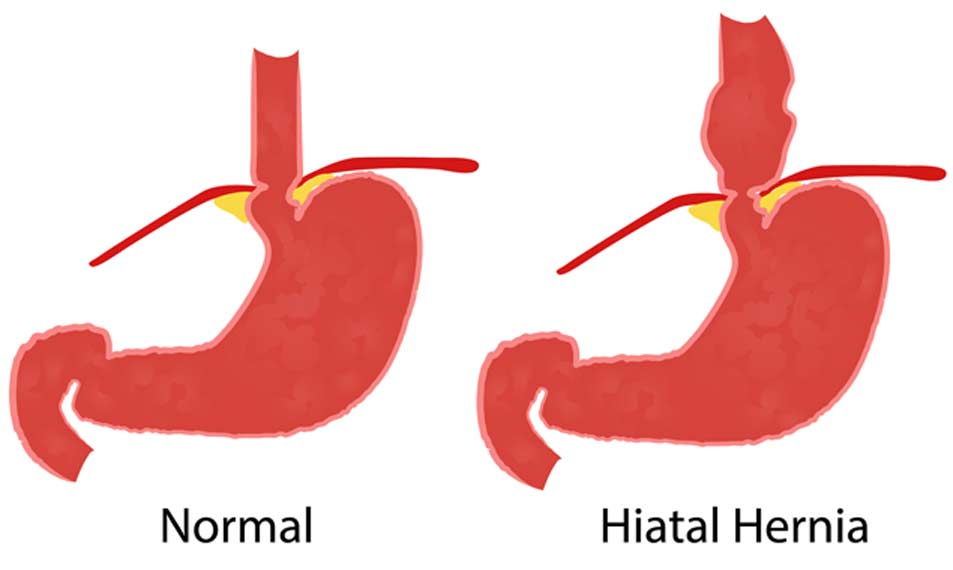
Types of Hiatal Hernias
Hiatal hernias can further be broken down into two more specific classifications: sliding hiatal hernias and paraesophageal (“fixed”) hernias. If the stomach and esophagus slide in and out of the chest through an opening, it’s the sliding type of hiatal hernia. With a fixed hernia of this nature, part of the stomach pushes through the diaphragm and remains there. A paraesophageal hernia is potentially more serious because blood flow to the stomach may become blocked.
Making a Diagnosis
Since chest pain could have other potential sources, such as peptic ulcers, chronic heartburn from other sources, or other upper abdominal issues, patients are advised to get an accurate diagnosis so the correct treatment can be recommended. Hiatal hernias may be diagnosed with an X-ray taken after a liquid with barium in it is consumed so the location of the stomach can be seen. Other times, diagnosis involves the insertion of a thin, lighted tube with a lens attached to it (endoscope) down the throat to the esophagus and stomach.
Symptom Management
It’s common for no treatment to be needed for hiatal hernias. Related symptoms such as acid reflux and heartburn are often treated with medication and diet changes that might include avoiding spicy foods, citrus fruits, caffeine, excessive amounts of alcohol, and foods/dishes made with tomatoes. Recommended medications may include over-the-counter antacids and prescription or OTC proton pump inhibitors and H2-receptor blockers.
Hiatal Hernia Surgery
Should medication prove to be ineffective, surgery may be discussed. Options include surgical rebuilding of weakened or thin esophageal muscles and repositioning of the stomach. If laparoscopic techniques are used, recovery time is usually shorter since smaller incisions are made.
It’s common for individuals with a hiatal hernia to have gastroesophageal reflux disease (GERD), although the two conditions aren’t directly related. As far as prevention goes, it’s not always possible to avoid having issues with a hiatal hernia. However, the risk of developing this particular type of hernia may be reduced by avoiding hard bowel movements, shedding excess pounds, and avoiding certain types of abdominal exercises that may be too strenuous.